In 2001, the Institute of Medicine (now the National Academy of Medicine) published a landmark paper,
Crossing the Quality Chasm, which laid out how the healthcare system has systematically fallen short in translating scientific research into medical practice. For instance, when I started at Flatiron, I was shocked to learn that even when potentially life-altering treatments are on the market, patients may not have access to that specific treatment, or their doctor may not have the information available to identify those treatment options.
Over the past 15 years, the healthcare industry has struggled to understand and address this breakdown. But two stories -- one a classic medical tale, the other from my own experience at Flatiron -- have helped me understand how technology can help bridge the gap between research and medical practice.
Ignaz Semmelweis and the worst product launch of all-time
A strange thing was happening in Vienna, Austria, in the late 1840s: pregnant women admitted to Vienna General Hospital were ten times more likely to die in childbirth if they were delivered by a doctor than if they were delivered by a midwife ( source: BMJ Quality & Safety ).
One staff obstetrician, Ignaz Semmelweis, became obsessed with understanding why this problem was occurring. After interviewing staff and shadowing doctors, Semmelweis began to notice a pattern: physicians were routinely performing autopsies and then treating patients. What's more, because blood on physicians' white coats was seen as a badge of honor, the physicians' clothing carried a high chance for infection.
[caption id="attachment_2134" align="aligncenter" width="317"] Ignaz Semmelweis[/caption]
Ignaz Semmelweis[/caption]
In the 1840s, the germ theory of disease had not yet been developed. But Semmelweis, a brilliant scientist, intuited that "cadaverous particles" from deceased patients were being transferred to pregnant mothers. So he performed an experiment: he had all the medical students in his ward sanitize their hands before delivering babies. As one might imagine, the maternal mortality rates in the ward quickly plummeted, from 18 percent to two percent.
Semmelweis had discovered one of the most powerful - and today, quite obvious - ideas in medicine: wash your hands.
In many ways, Semmelweis had been operating in classic startup mode. He had a brilliant insight (infection causes illness, sometimes death), created a beta product (handwashing), and then validated it with customers (medical students and their patients). At this stage, Semmelweis must have assumed that the path from research into medical practice was simple: announce his findings, and change the world.
But it didn't happen that way. And it didn't because Semmelweis did not consider his product launch strategy.
What did he do wrong?
Ultimately, it took thirty years for the medical community to embrace antiseptic treatment. And in that time, in part because of Semmelweis' poor execution, the medical community continued a practice that was detrimental to patient care.
Navigating quality measures at Flatiron
At Flatiron, our mission places our products at the intersection between healthcare and technology, and requires us to confront many of the same challenges Semmelweis faced two centuries earlier. One of our product initiatives involves supporting oncology practices as they navigate new value-based care models: a system in which providers are reimbursed based on the quality and affordability of care provided, not the number of health care services they deliver.
In 2016, a few of us began building a product for Flatiron practices that were participating in the Oncology Care Model (OCM), one such value-based care program. When a practice participates in the OCM, they are required to track and report on specific clinical quality metrics in order to be reimbursed for the care that they provide. We knew that for this product to be successful, we would have to find ways to help them improve their quality of care and track their progress.
So we embarked on a series of visits to clinics, centering our conversations around a central question: how can we help practices improve their quality of care? After interviewing physicians and practice administrators, we began to notice a pattern: doctors are competitive , and scoring them next to their peers could incentivize quality improvement.
Our user research was informed by industry-wide product and design principles and best practices, and we developed the product using Agile methodologies, a common software development practice at many startups that favors quick iteration cycles and tight feedback loops. We drew upon all of this to build an automated physician quality measure dashboard -- all within a few weeks:
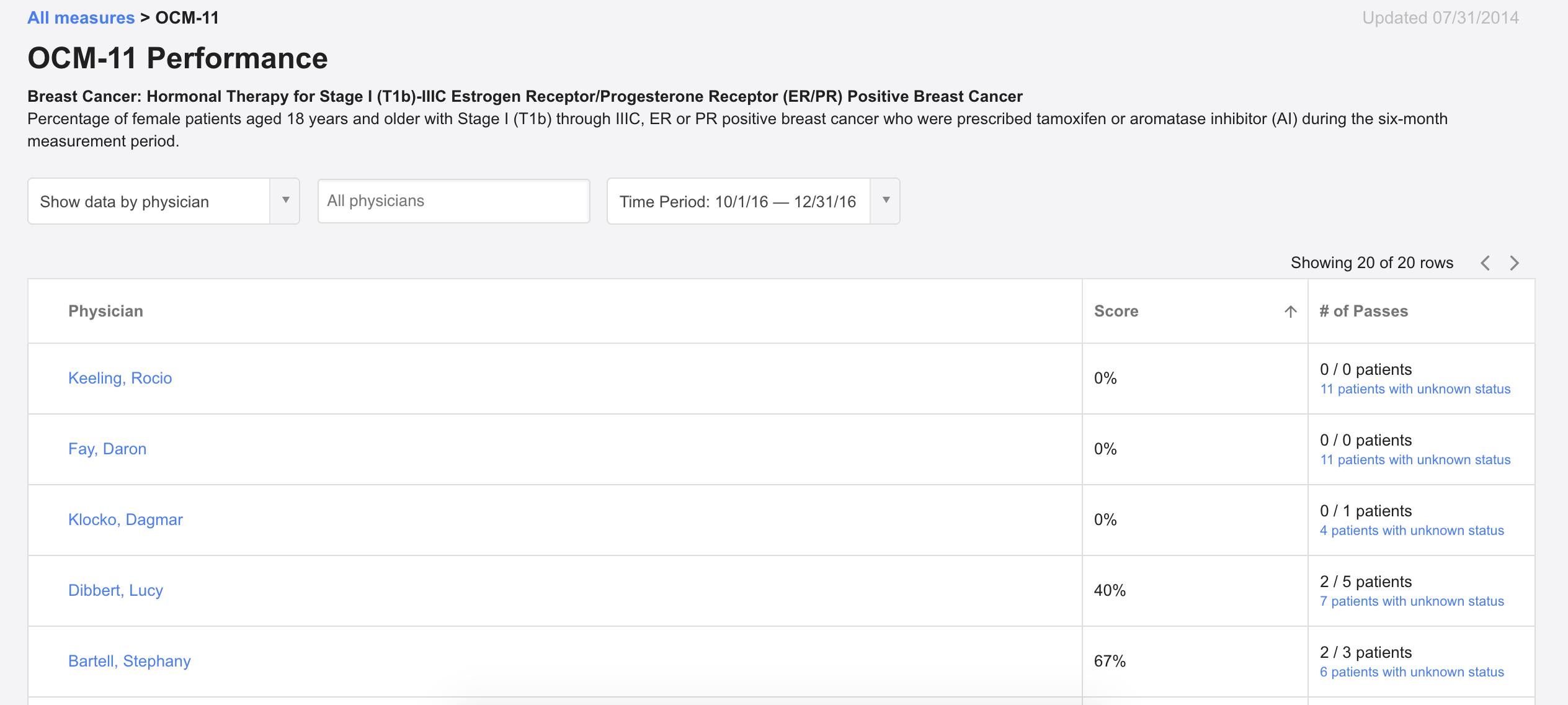
If you look at the above screenshot closely, you might see the major flaw: in many instances, our dashboard produced zero results.
Why? Key elements of patients' care are often not documented in structured fields within an electronic health record (EHR). In many cases, the patient information needed to calculate a quality measure (in the image above, for Stage I-IIIC ER/PR positive breast cancer patients) can live in unstructured text, handwritten notes, labs, or scanned documents attached within the EHR. This disparate data made it difficult to reliably automatically calculate performance for any physician.
Crossing the chasm
In some ways, our team made the same mistake Semmelweis did: we initially assumed that a great idea (quality measure improvement within value-based care) would yield a great product and user adoption. We've now realized that our dashboard was only the start in identifying the messy ways in which new research and technologies are incorporated into medical practice. Much like the quality chasm in healthcare, we face a similar chasm as a technology company -- the one between product launch and adoption.
Our experience with our practices in the OCM has informed how we think technology and healthcare can cross chasms together. We are investing in EHR workflows that make it easier for providers to treat their patients and track the results; and in data processing tools that will enable providers and researchers to make sense of this data. In oncology, this means we are building towards what Dr. Amy Abernethy, our Chief Medical and Scientific Officer, coined as a learning healthcare system , where every cancer patient's treatment is informed by previous patients' experiences; and each patient's experience informs future treatment and research.
What is just as true of nineteenth-century Vienna as today is that this process only works with humility and true partnership. When a doctor launches a product, or when technologists enter an oncology practice, there is much we can learn from each other in building a system that does justice to the patients it serves.
This story was first presented as part of Fast Company's Innovation Festival. Read more here .
Over the past 15 years, the healthcare industry has struggled to understand and address this breakdown. But two stories -- one a classic medical tale, the other from my own experience at Flatiron -- have helped me understand how technology can help bridge the gap between research and medical practice.
Ignaz Semmelweis and the worst product launch of all-time
A strange thing was happening in Vienna, Austria, in the late 1840s: pregnant women admitted to Vienna General Hospital were ten times more likely to die in childbirth if they were delivered by a doctor than if they were delivered by a midwife ( source: BMJ Quality & Safety ).
One staff obstetrician, Ignaz Semmelweis, became obsessed with understanding why this problem was occurring. After interviewing staff and shadowing doctors, Semmelweis began to notice a pattern: physicians were routinely performing autopsies and then treating patients. What's more, because blood on physicians' white coats was seen as a badge of honor, the physicians' clothing carried a high chance for infection.
[caption id="attachment_2134" align="aligncenter" width="317"]
 Ignaz Semmelweis[/caption]
Ignaz Semmelweis[/caption]
In the 1840s, the germ theory of disease had not yet been developed. But Semmelweis, a brilliant scientist, intuited that "cadaverous particles" from deceased patients were being transferred to pregnant mothers. So he performed an experiment: he had all the medical students in his ward sanitize their hands before delivering babies. As one might imagine, the maternal mortality rates in the ward quickly plummeted, from 18 percent to two percent.
Semmelweis had discovered one of the most powerful - and today, quite obvious - ideas in medicine: wash your hands.
In many ways, Semmelweis had been operating in classic startup mode. He had a brilliant insight (infection causes illness, sometimes death), created a beta product (handwashing), and then validated it with customers (medical students and their patients). At this stage, Semmelweis must have assumed that the path from research into medical practice was simple: announce his findings, and change the world.
But it didn't happen that way. And it didn't because Semmelweis did not consider his product launch strategy.
What did he do wrong?
- Semmelweis attacked physicians. He told them they were killing their patients, and he took every chance he could to publicly berate doctors and shame them into handwashing.
- Semmelweis believed that his results were self-evident, so he didn't publish his evidence for thirteen years. When he finally published a written manuscript on antiseptic treatment, it was incoherent and mainly attacked doctors yet again.
- Semmelweis was a natural outsider: a Hungarian Jew in Catholic Austria; an obstetrician in a research community of surgeons. But more than that, he was deeply stubborn, and none of his peers liked him. Semmelweis never found allies in the medical field.
Ultimately, it took thirty years for the medical community to embrace antiseptic treatment. And in that time, in part because of Semmelweis' poor execution, the medical community continued a practice that was detrimental to patient care.
Navigating quality measures at Flatiron
At Flatiron, our mission places our products at the intersection between healthcare and technology, and requires us to confront many of the same challenges Semmelweis faced two centuries earlier. One of our product initiatives involves supporting oncology practices as they navigate new value-based care models: a system in which providers are reimbursed based on the quality and affordability of care provided, not the number of health care services they deliver.
In 2016, a few of us began building a product for Flatiron practices that were participating in the Oncology Care Model (OCM), one such value-based care program. When a practice participates in the OCM, they are required to track and report on specific clinical quality metrics in order to be reimbursed for the care that they provide. We knew that for this product to be successful, we would have to find ways to help them improve their quality of care and track their progress.
So we embarked on a series of visits to clinics, centering our conversations around a central question: how can we help practices improve their quality of care? After interviewing physicians and practice administrators, we began to notice a pattern: doctors are competitive , and scoring them next to their peers could incentivize quality improvement.
Our user research was informed by industry-wide product and design principles and best practices, and we developed the product using Agile methodologies, a common software development practice at many startups that favors quick iteration cycles and tight feedback loops. We drew upon all of this to build an automated physician quality measure dashboard -- all within a few weeks:

If you look at the above screenshot closely, you might see the major flaw: in many instances, our dashboard produced zero results.
Why? Key elements of patients' care are often not documented in structured fields within an electronic health record (EHR). In many cases, the patient information needed to calculate a quality measure (in the image above, for Stage I-IIIC ER/PR positive breast cancer patients) can live in unstructured text, handwritten notes, labs, or scanned documents attached within the EHR. This disparate data made it difficult to reliably automatically calculate performance for any physician.
Crossing the chasm
In some ways, our team made the same mistake Semmelweis did: we initially assumed that a great idea (quality measure improvement within value-based care) would yield a great product and user adoption. We've now realized that our dashboard was only the start in identifying the messy ways in which new research and technologies are incorporated into medical practice. Much like the quality chasm in healthcare, we face a similar chasm as a technology company -- the one between product launch and adoption.
Our experience with our practices in the OCM has informed how we think technology and healthcare can cross chasms together. We are investing in EHR workflows that make it easier for providers to treat their patients and track the results; and in data processing tools that will enable providers and researchers to make sense of this data. In oncology, this means we are building towards what Dr. Amy Abernethy, our Chief Medical and Scientific Officer, coined as a learning healthcare system , where every cancer patient's treatment is informed by previous patients' experiences; and each patient's experience informs future treatment and research.
What is just as true of nineteenth-century Vienna as today is that this process only works with humility and true partnership. When a doctor launches a product, or when technologists enter an oncology practice, there is much we can learn from each other in building a system that does justice to the patients it serves.
This story was first presented as part of Fast Company's Innovation Festival. Read more here .


